This lung disease from the 1800’s has begun to reappear again, especially among the elderly. Historically cases were due to untreated chest infections where antibiotics weren’t readily available and the poorer part of the community suffered with it more.
Research data from the NHS shows that of the 12000 patients admitted with Bronchiectasis in 2013-2014 most of them were over 60 years of age. Cases have doubled in the last decade among those aged 70 and over and now more than 1 in every 100 in this category will be affected.
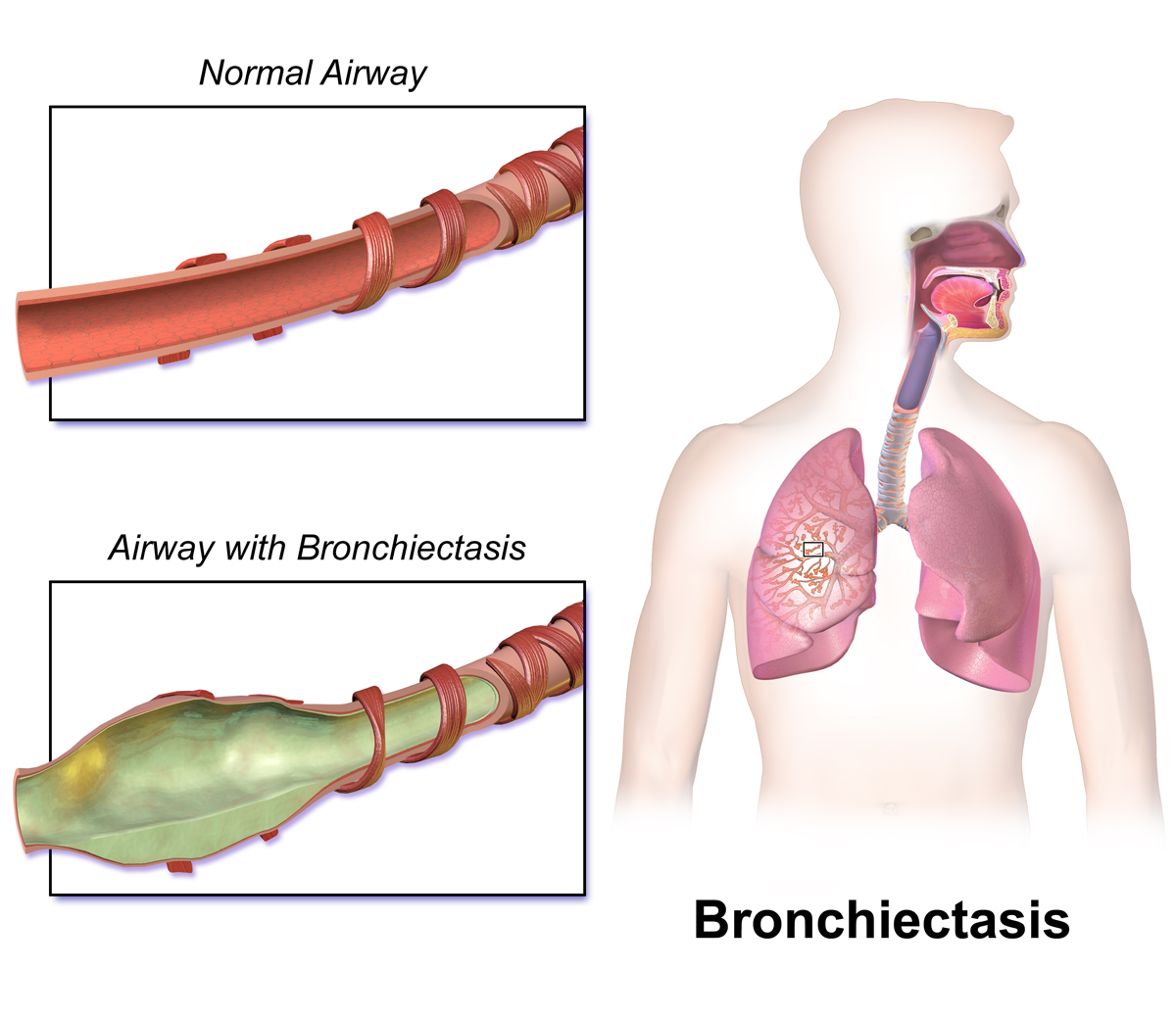
Bronchiectasis occurs when the airways of the lungs become abnormally widened, which results in chronic inflammation due to the inability to clear mucus secretions in the airway passages leading to a build-up of mucus. The excess mucus also harbours bacteria which can lead to worsening of the condition due to frequent infections. Symptoms typically include a chronic cough, shortness of breath, wheezing, fatigue, coughing up blood, and chest pain, along with worsening respiratory function. Inhaled antibiotics, bronchodilators, physical methods of dislodging mucus and oxygen therapy are all part of the treatment for this disease.
Experts agree that bronchiectasis may occur in people who suffered an infection in childhood such as pneumonia or whooping cough, which damage the lung. Underlying problems with the immune system and allergies are also thought to play a role. This is a main factor as to why the elderly are susceptible as with age comes a compromised immune system.
Bronchiectasis tends to occur as an after-effect of a chest infection such as whooping cough, tuberculosis, pneumonia or measles – particularly if the infection was not treated with antibiotics. Damage to the bronchi takes years to build up and symptoms don’t tend to start until middle age, even if the original infection was years earlier.
‘Antibiotics only really came in on a regular basis in the Sixties and Seventies,’ says Professor Brown.’But we also see people who had antibiotics and despite that have bronchiectasis. Even if you treat it, the infection can still cause scarring, it’s just less likely.’
The disease is incurable and although infections can be treated with antibiotics, there are concerns that the bacteria is becoming resistant to drugs.
Surprisingly more women are affected than men for no known reason other than for the fact that rheumatoid arthritis is a high risk factor for developing Bronchiectasis and this condition is more common in women. Also patients tend to be more affluent. ‘We found the disease has had a resurgence in recent years, particularly among more well-off members of society,’ says Jeremy Brown, a professor of respiratory infection at University College London. ‘It could be partly down to improved diagnosis in these groups, but whatever the reason we need better treatment options.’
The study found that 42% of people with bronchiectasis also had asthma and 36% had chronic obstructive pulmonary disease (COPD). This is an important finding and can help with long-term management of these conditions. A study has found that COPD can be predictive of developing Bronchiectasis but that also this then makes the outcome for the COPD patient a lot graver.
The reasons for this disease increasing in certain groups is being investigated but it could be that it is running alongside the fact that diagnosis for other predictive diseases like COPD has improved in recent years but as to the reason why it is more prevalent in middle-class patients is unknown. With this rise of cases in recent years more research is now underway to improve treatment and to investigate the disease’s coexistence with other diseases such as COPD.
References: http://home.bt.com and http://bronchiectasisnewstoday.com and http://www.dailymail.co.uk
1 Comment
Add comment Cancel reply
You must be logged in to post a comment.





Here is a site where researchers are doing surveys about bronchiectasis. If you have the disease, please check it out. You may be able to help researchers by doing this survey. https://www.surveymonkey.com/r/Bronchsurvey2016